Managing Trauma's Impact on Schizophrenia: A Practical Guide is a comprehensive resource aimed at healthcare professionals, therapists, and individuals living with schizophrenia.
This practical guide delves into the intricate relationship between trauma and schizophrenia, providing valuable insights and evidence-based strategies for effectively managing trauma-related symptoms in individuals with schizophrenia.
Drawing on a wealth of research and clinical experience, this guide offers a clear understanding of how trauma impacts the course and treatment of schizophrenia.
It explores the signs and symptoms of trauma in schizophrenia, provides guidance on incorporating trauma-focused approaches into treatment plans, and equips readers with coping strategies to alleviate trauma-related symptoms.
By emphasizing resilience-building techniques, this guide empowers individuals with schizophrenia to navigate the challenges of trauma and embark on a path towards healing.
Understanding the Trauma-Schizophrenia Connection
The connection between trauma and schizophrenia is frequently observed and extensively researched in the field of mental health. There is a growing body of evidence that suggests a significant association between traumatic experiences and the development or exacerbation of schizophrenia symptoms. Trauma can refer to a wide range of experiences, including physical or sexual abuse, neglect, emotional trauma, or witnessing or experiencing a life-threatening event.
Research has found that individuals with schizophrenia are more likely to have experienced trauma compared to those without the disorder. For example, a study conducted by Read et al. (2005) found that approximately 75% of individuals diagnosed with schizophrenia had experienced at least one traumatic event in their lifetime. Furthermore, trauma may also contribute to a more severe and chronic course of the illness, as well as increased rates of comorbid conditions such as post-traumatic stress disorder (PTSD) or substance abuse.
The exact mechanisms underlying the trauma-schizophrenia connection are still being investigated. It is thought that trauma may interact with genetic and neurobiological factors to increase the risk of developing schizophrenia or worsen existing symptoms. Additionally, trauma may lead to changes in cognitive functioning, emotion regulation, and social functioning, all of which are relevant to the manifestation and course of schizophrenia.
Understanding the trauma-schizophrenia connection is crucial for clinicians and researchers alike. By addressing and treating trauma in individuals with schizophrenia, it may be possible to improve outcomes and enhance overall well-being.
Recognizing the Signs and Symptoms of Trauma in Schizophrenia
Researchers and clinicians must be able to identify the signs and symptoms of trauma in individuals with schizophrenia in order to effectively manage its impact. Trauma can have a profound impact on individuals with schizophrenia, exacerbating symptoms and hindering recovery. However, recognizing trauma in this population can be challenging due to the overlap of symptoms between schizophrenia and trauma-related disorders.
Some common signs and symptoms of trauma in individuals with schizophrenia include:
- Intrusive thoughts or memories related to the traumatic event
- Hypervigilance
- Heightened startle response
- Flashbacks
- Nightmares
- Avoidance of triggers associated with the trauma
Additionally, individuals may experience emotional numbing, dissociation, irritability, and difficulties with concentration and sleep.
Clinicians should also be aware of the potential impact of trauma on treatment adherence and engagement. Trauma may contribute to increased treatment resistance, mistrust, and difficulties in forming therapeutic relationships. It is essential for clinicians to create a safe and supportive environment to address trauma-related issues and incorporate trauma-informed care into the treatment plan.
Validated assessment tools, such as the Clinician-Administered PTSD Scale for DSM-5 (CAPS-5), can aid in the identification and diagnosis of trauma in individuals with schizophrenia. Collaborative and multidisciplinary approaches involving psychiatrists, psychologists, social workers, and trauma specialists are crucial in effectively managing trauma's impact on schizophrenia.
Addressing Trauma in Schizophrenia Treatment
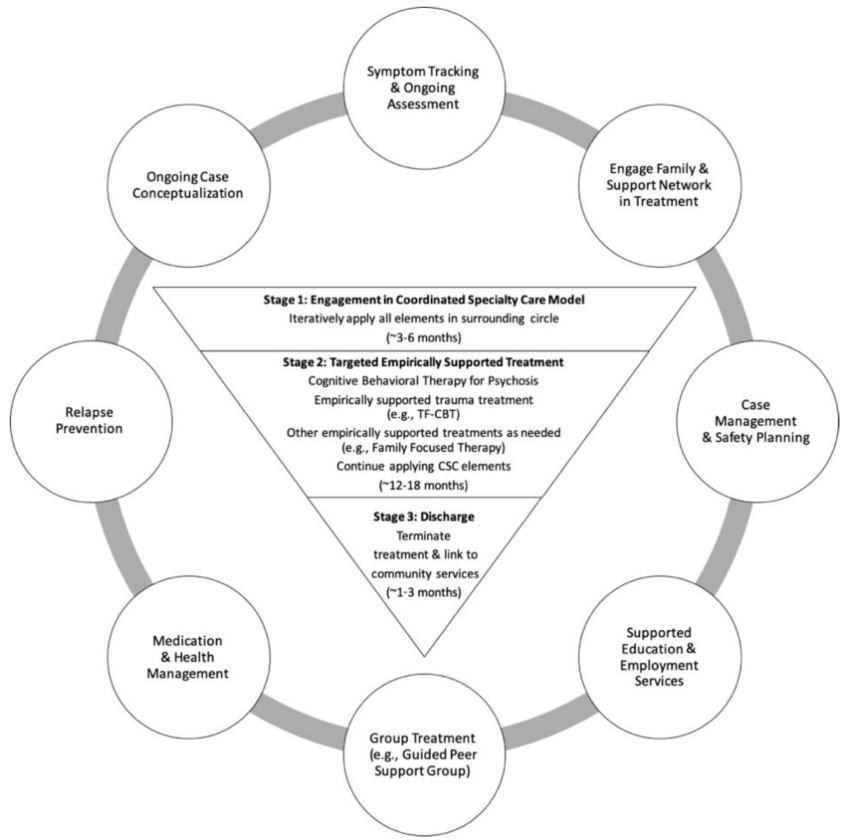
Addressing trauma in schizophrenia treatment requires a comprehensive and integrated approach that acknowledges the impact of trauma on symptomatology and recovery. Trauma can have a profound effect on individuals with schizophrenia, exacerbating their symptoms and hindering their ability to engage in treatment effectively. Therefore, it is crucial for mental health professionals to incorporate trauma-informed practices into their treatment plans.
One important aspect of addressing trauma in schizophrenia treatment is psychoeducation. Patients need to understand the connection between their traumatic experiences and their symptoms. Providing them with information about trauma and its impact on mental health can help reduce shame, guilt, and self-blame commonly associated with trauma. Additionally, it can empower patients to actively participate in their treatment and recovery process.
Another crucial component of trauma-informed care is the use of evidence-based therapies, such as trauma-focused cognitive-behavioral therapy (TF-CBT) and eye movement desensitization and reprocessing (EMDR). These therapies aim to help individuals process traumatic memories and develop coping strategies to manage trauma-related symptoms. By addressing trauma directly, these therapies can alleviate distress and improve overall functioning in individuals with schizophrenia.
Furthermore, it is essential to create a safe and supportive treatment environment. This involves establishing trust, promoting open communication, and ensuring that the treatment environment is free from retraumatization. Mental health professionals should practice active listening, validate patients' experiences, and provide empathy and support throughout the treatment process.
Implementing Coping Strategies for Trauma-related Symptoms in Schizophrenia
Implementing coping strategies for trauma-related symptoms in schizophrenia can be a pivotal aspect of treatment. Trauma can significantly impact individuals with schizophrenia, exacerbating their symptoms and affecting their overall well-being. By incorporating coping strategies specifically tailored to address trauma-related symptoms, clinicians can help patients better manage their condition and improve their quality of life.
There are several evidence-based coping strategies that have shown promise in the treatment of trauma-related symptoms in schizophrenia. These strategies aim to help individuals effectively cope with distressing experiences and reduce the impact of trauma on their daily functioning.
One such strategy is cognitive-behavioral therapy (CBT), which focuses on identifying and changing negative thought patterns and behaviors associated with trauma. CBT has been shown to be effective in reducing symptoms of post-traumatic stress disorder (PTSD) in individuals with schizophrenia.
Another strategy is mindfulness-based interventions, which involve cultivating present-moment awareness and non-judgmental acceptance of one's experiences. Mindfulness techniques can help individuals with schizophrenia develop greater emotional regulation and reduce the distressing effects of trauma.
In addition, social support and psychoeducation play a crucial role in coping with trauma-related symptoms. Supportive environments and education about trauma and its impact can empower individuals with schizophrenia to better understand their experiences and develop effective coping strategies.
Implementing these coping strategies as part of a comprehensive treatment plan can help individuals with schizophrenia better manage trauma-related symptoms and improve their overall well-being. It is important for clinicians to tailor these strategies to each individual's unique needs and provide ongoing support and guidance throughout the treatment process.
| Coping Strategy | Description | Evidence |
|---|---|---|
| Cognitive-Behavioral Therapy (CBT) | Focuses on identifying and changing negative thought patterns and behaviors associated with trauma. | Effective in reducing symptoms of PTSD in individuals with schizophrenia. |
| Mindfulness-Based Interventions | Involves cultivating present-moment awareness and non-judgmental acceptance of one's experiences. | Can help develop emotional regulation and reduce the distressing effects of trauma in schizophrenia. |
| Social Support | Provides a supportive environment and education about trauma and its impact. | Can empower individuals to better understand their experiences and develop effective coping strategies. |
Building Resilience and Healing From Trauma in Schizophrenia
Individuals with schizophrenia who have experienced trauma can benefit from building resilience and finding healing strategies tailored to their unique needs and experiences. Trauma can have a profound impact on individuals with schizophrenia, exacerbating symptoms and impairing overall functioning. However, with the right support and interventions, individuals can develop resilience and work towards healing from their traumatic experiences.
Here are four strategies that can help individuals with schizophrenia build resilience and find healing:
- Psychoeducation: Providing individuals with knowledge about trauma and its effects can empower them to make sense of their experiences and develop coping mechanisms. Psychoeducation can also reduce stigma and enhance treatment engagement.
- Trauma-focused therapy: Therapies such as Cognitive Processing Therapy (CPT) and Eye Movement Desensitization and Reprocessing (EMDR) have shown promise in treating trauma in individuals with schizophrenia. These therapies help individuals process traumatic memories and develop more adaptive beliefs and coping strategies.
- Social support: Building a supportive network of family, friends, and peers can provide a sense of belonging and emotional validation. Social support can also provide opportunities for individuals to share their experiences and receive encouragement and understanding.
- Self-care practices: Engaging in self-care activities, such as exercise, meditation, and creative outlets, can help individuals manage stress, promote emotional well-being, and enhance resilience. Encouraging individuals to prioritize self-care can be an essential part of the healing process.
Frequently Asked Questions
What Are Common Triggers for Trauma in Individuals With Schizophrenia?
Common triggers for trauma in individuals with schizophrenia can include experiences of childhood abuse, neglect, or trauma, as well as ongoing stressors such as interpersonal conflicts, social isolation, and hospitalizations. These triggers can exacerbate symptoms and impact overall mental health.
How Does Trauma Impact Medication Adherence in Individuals With Schizophrenia?
Trauma can negatively impact medication adherence in individuals with schizophrenia. The experience of trauma can lead to increased symptoms, such as anxiety and distrust, which may make it difficult for individuals to consistently take their medication as prescribed.
Are There Any Specific Therapies or Treatment Approaches That Are More Effective in Addressing Trauma in Individuals With Schizophrenia?
While there is limited research on specific therapies or treatment approaches for addressing trauma in individuals with schizophrenia, some evidence suggests that trauma-focused cognitive behavioral therapy (TF-CBT) may be effective in reducing trauma-related symptoms in this population.
How Can Family Members and Loved Ones Support an Individual With Schizophrenia Who Has Experienced Trauma?
Family members and loved ones can support individuals with schizophrenia who have experienced trauma by providing a supportive and understanding environment, encouraging professional help-seeking, and promoting self-care strategies such as healthy coping mechanisms and stress reduction techniques.
Can Trauma Worsen the Prognosis or Overall Course of Schizophrenia?
Trauma can potentially worsen the prognosis or overall course of schizophrenia. Research suggests that individuals with schizophrenia who have experienced trauma may have more severe symptoms, higher rates of relapse, and poorer functional outcomes compared to those without trauma exposure.