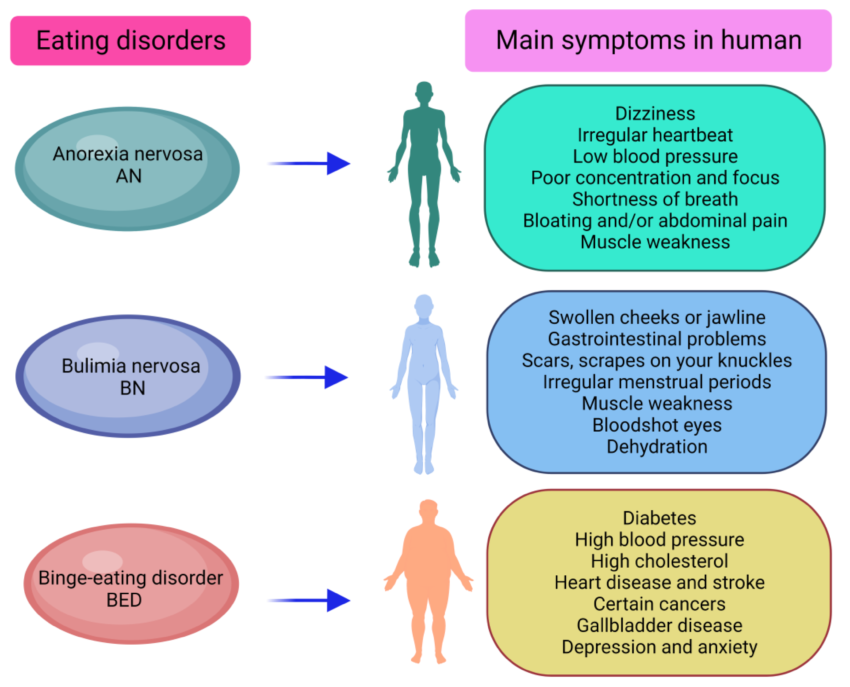
Eating disorders are complex mental illnesses that affect millions of individuals worldwide. While various factors contribute to their development, recent research has highlighted the significant role of genetics in shaping susceptibility to these disorders.
This introduction aims to examine the three most influential genetic factors in eating disorder development, shedding light on their implications for understanding and treating these conditions. By understanding the genetic underpinnings of eating disorders, researchers and clinicians can better identify individuals at risk, design targeted interventions, and develop personalized treatment plans.
Through a professional lens, this concise overview will explore the latest scientific findings, emphasizing the importance of genetics in unraveling the complexities of eating disorders and paving the way for improved prevention and management strategies.
Genetic Influences on Eating Disorders
There are several prominent genetic factors that contribute to the development of eating disorders. Research has shown that genetic influences play a significant role in the development of eating disorders such as anorexia nervosa, bulimia nervosa, and binge eating disorder. Twin and family studies have consistently demonstrated that individuals with a family history of an eating disorder are at a higher risk of developing the disorder themselves.
One of the main genetic factors implicated in eating disorders is heritability. Studies have shown that the heritability of eating disorders ranges from 28% to 83%, indicating a strong genetic component. This means that genetic factors contribute significantly to the risk of developing an eating disorder.
Furthermore, specific genes have been associated with an increased susceptibility to eating disorders. For example, variations in genes involved in serotonin, dopamine, and the brain-derived neurotrophic factor (BDNF) have been linked to an increased risk of developing an eating disorder. These genes are involved in regulating mood, reward, and appetite, which are all key factors in the development of eating disorders.
Understanding the genetic factors involved in eating disorders is crucial for early detection, prevention, and treatment. By identifying individuals who are genetically predisposed to developing an eating disorder, interventions can be implemented earlier, potentially reducing the severity and chronicity of the disorder.
Additionally, this knowledge can inform the development of targeted therapies that take into account an individual's genetic profile, improving treatment outcomes and long-term recovery.
Key Genetic Factors in Eating Disorder Development
Several significant genetic factors have been identified in the development of eating disorders. Research has shown that genetic factors play a crucial role in determining an individual's susceptibility to developing an eating disorder. One key genetic factor is the heritability of eating disorders, which indicates the degree to which genetic factors contribute to the development of these disorders. Twin studies have found that genetic factors account for approximately 40-60% of the variance in eating disorder symptoms, suggesting a strong genetic component.
Another important genetic factor is the involvement of specific genes related to appetite regulation and body weight regulation. Studies have identified certain genes, such as the melanocortin-4 receptor (MC4R) gene, the leptin gene, and the brain-derived neurotrophic factor (BDNF) gene, that are associated with an increased risk of developing eating disorders. These genes are involved in the regulation of hunger, satiety, and body weight, and variations in these genes may disrupt these processes, leading to the development of disordered eating behaviors.
Additionally, genetic factors related to personality traits, such as impulsivity and perfectionism, have also been implicated in the development of eating disorders. Certain genetic variations may influence an individual's susceptibility to these personality traits, which in turn may increase the risk of developing disordered eating patterns.
It is important to note that while genetic factors play a significant role in the development of eating disorders, they do not act alone. Environmental factors, such as societal pressures, family dynamics, and traumatic experiences, also contribute to the development of these disorders. Understanding the interplay between genetic and environmental factors is crucial for developing effective prevention and treatment strategies for individuals with eating disorders.
The Role of Genetics in Eating Disorders
The role of genetics in eating disorders is crucial and has been extensively studied to understand the underlying factors contributing to the development of these disorders. Research suggests that genetic factors contribute significantly to the risk of developing an eating disorder. Here are four key points that shed light on the role of genetics in eating disorders:
- Heritability: Studies have shown that there is a genetic component to eating disorders, with heritability estimates ranging from 40% to 80%. This means that a significant proportion of the risk for developing an eating disorder can be attributed to genetic factors.
- Genetic variations: Certain genes have been associated with an increased susceptibility to eating disorders, including genes involved in appetite regulation, metabolism, and brain function. These genetic variations may influence an individual's vulnerability to developing disordered eating behaviors.
- Gene-environment interaction: While genetics play a significant role, it is important to note that eating disorders develop as a result of complex interactions between genetic and environmental factors. Adverse life events, social pressures, and cultural influences can interact with genetic predispositions, increasing the risk of developing an eating disorder.
- Understanding the biological pathways: Studying the role of genetics in eating disorders can help researchers uncover the biological pathways that contribute to the development of these disorders. This knowledge can potentially lead to the development of more effective prevention and treatment strategies, tailored to individuals based on their genetic profiles.
Frequently Asked Questions
What Are Some Non-Genetic Factors That Contribute to the Development of Eating Disorders?
Non-genetic factors that contribute to the development of eating disorders include societal pressure, body dissatisfaction, perfectionism, low self-esteem, history of trauma, and dysfunctional family dynamics. These factors interact with genetic predisposition to increase vulnerability.
Are Eating Disorders Solely Caused by Genetics?
While genetic factors play a significant role in the development of eating disorders, it is crucial to understand that they are not the sole cause. Environmental, psychological, and social factors also contribute to the complex etiology of eating disorders.
How Do Genetic Factors Interact With Environmental Factors in the Development of Eating Disorders?
Genetic factors play a significant role in the development of eating disorders, but they do not act alone. The interaction between genetic and environmental factors is crucial in understanding the complex etiology of these disorders.
Can Genetic Factors Be Used to Predict or Prevent the Development of Eating Disorders?
Genetic factors can provide valuable insights into the prediction and prevention of eating disorders. For instance, a hypothetical case study could explore how identifying specific gene variants associated with disordered eating behaviors could inform targeted intervention strategies for at-risk individuals.
Are There Specific Genetic Markers or Mutations That Have Been Identified as Risk Factors for Eating Disorders?
Specific genetic markers or mutations that have been identified as risk factors for eating disorders include variations in the FTO, BDNF, and MC4R genes. However, it is important to note that these factors alone do not determine the development of eating disorders.